Portal, AZ - Rodeo, NM
Serving The Communities Of Portal and Rodeo (www.portal-rodeo.com)
Serving The Communities Of Portal and Rodeo (www.portal-rodeo.com)

Ticks -Don’t Get Ticked Off
According to the CDC tick season really is off to an unusually bad start. Emergency department visits for tick bites are running at nearly triple the typical rate at this time of year. The Northeast is bearing the brunt of it, with the Midwest running a close second. There are about 2 dozen species in Arizona, though only a few commonly bite humans and spread disease.
Let’s start with one species that is getting a lot of press lately, even if it is not typically (YET) present in Arizona: the Lone Star Tick. The bite causes a meat allergy. The tick introduces a sugar molecule called alpha-gal into your bloodstream. Your immune system responds. The next time you eat red meat, your body reacts. Beef, pork, lamb, and venison are the main triggers. Sensitivity varies a lot, which is part of why it’s so hard to diagnose. Some people regain tolerance if they avoid further tick bites. Others don’t recover. No treatment exists beyond avoidance. You can see from the distribution map it is spreading. There are now a few sporadic cases recently reported in New Mexico (and even a few SUSPECTED cases in Arizona).

It’s Spring: Warm Weather And The Ticks Are Here

Lone Star Tick - Female
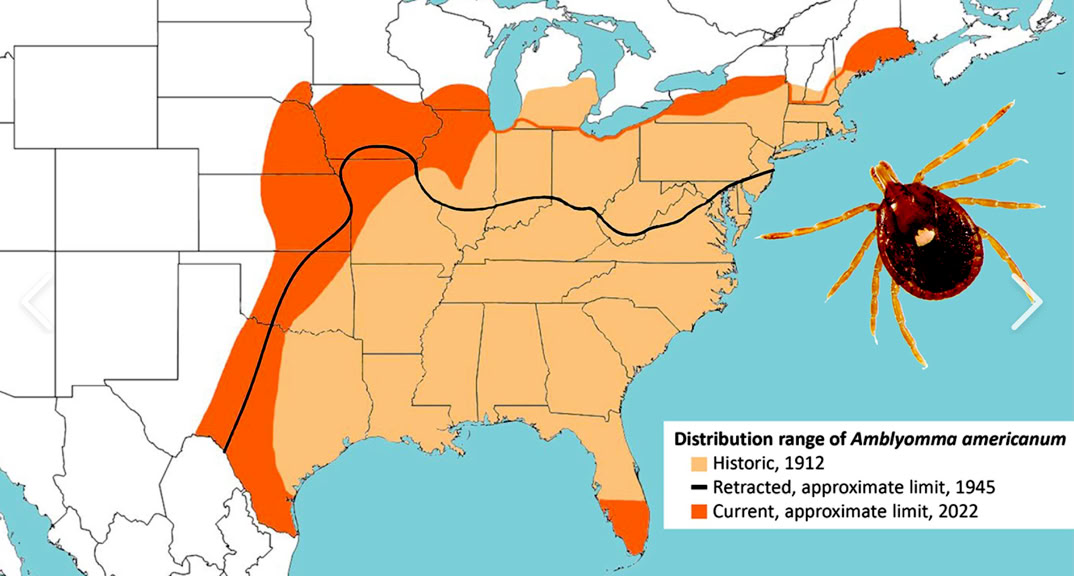
Brown Dog Tick - This is the BAD one
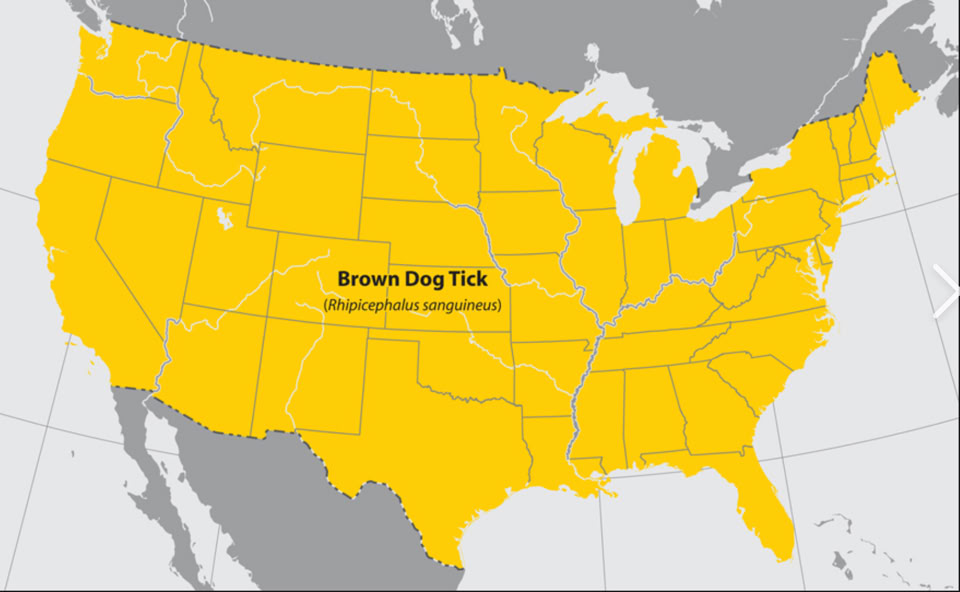
Where is this tick found? EVERYWHERE! It is one of the few ticks that can complete all life stages inside homes and survives in comparatively dry indoor settings by sheltering in microcracks and emerging to feed when conditions/hosts are favorable.
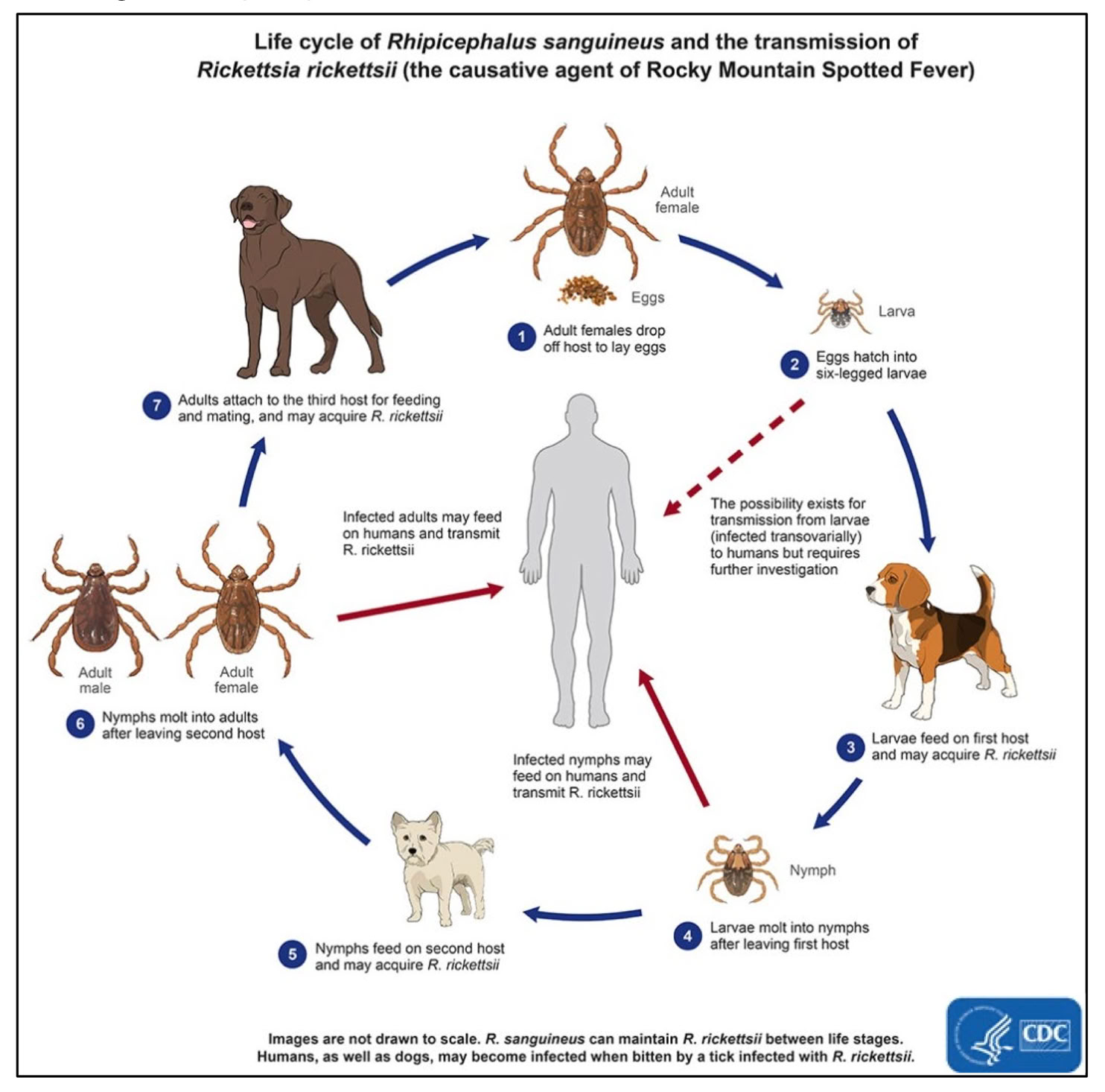
While human bites are rare, they do occur, especially in homes or kennels with infested dogs. The most serious risk is Rocky Mountain spotted fever (RMSF), caused by the bacterium Rickettsia rickettsii. Symptoms can include fever, headache, rash (often starting on wrists/ankles), muscle aches, and nausea. Without prompt antibiotic treatment, RMSF can be life-threatening. In Arizona, the Brown Dog Tick is the primary vector of RMSF
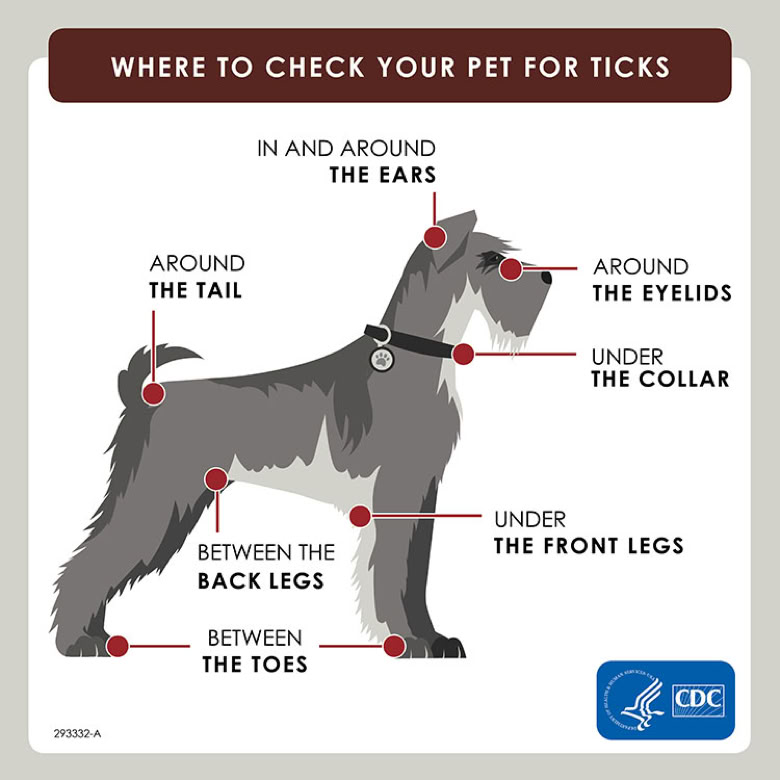
Identifying a brown dog tick is crucial for the health of your pet. Regularly checking your dog for ticks, especially in areas where they are likely to attach, is essential for prevention and early detection. If you suspect your dog has been bitten by a tick, consult your veterinarian for advice and treatment options.

Brown Dog Tick
Wear light-colored, long-sleeved shirts and pants to easily spot ticks and reduce skin exposure.
Tuck your pants into your socks and your shirt into your pants to block ticks from reaching your skin.
Apply EPA-registered insect repellents containing DEET, picaridin, or IR3535 to exposed skin and clothing.
Treat clothing and gear with permethrin or purchase pre-treated items for added protection.
Stick to cleared paths or trails and avoid walking through tall grass, brush, or leaf litter.
Check your clothing, gear, and pets for ticks before entering your home.
Tumble dry clothes on high heat for 10 minutes to kill ticks. If clothes are damp, dry them longer. Wash clothes in hot water if needed.
Shower within two hours of being outdoors to wash off unattached ticks and perform a full-body tick check.
Inspect your body, especially areas like underarms, behind knees, around the waist, and in the hairline, using a mirror if necessary.
Maintain your yard by mowing the lawn, removing leaf litter, and clearing tall grass. Create a 3-ft barrier of wood chips or gravel between lawns and wooded areas.